National Patient Safety Goals: A Glimpse At 2025
In 2002 The Joint Commission (TJC) first established the National Patient Safety Goals (NPSG) Program. In 2003, TJC rolled out the first set of NPSG’s. Each year, TJC prioritizes patient safety goals for various healthcare programs. The goals are prioritized based upon feedback from healthcare providers, stakeholders, purchasers and consumer groups. The intent is to minimize risk to patients. With each goal that is identified, there are also essentials steps detailing how to address each goal to meet a desirable outcome for patients. For healthcare organizations who are accredited by TJC, their accreditation status highly depends on a facilities commitment to meeting NPSG’s with success.
For healthcare organizations who are accredited or who are seeking accreditation by TJC, it is important to stay current with the updated goals each year. Of note, many of the goals that are identified do not change drastically from year to year. This is largely because we continue to see adverse outcomes surrounding the same issues each year in the healthcare industry.
If you are or are planning on becoming a TJC accredited organization, it is imperative that you remain current with each year’s set of established goals. Be sure to update this information throughout your facility. Regardless of the type of healthcare program you have, TJC issues a simplified version of each of the goals sets which can be easily printed off their website and used for team education and promoting awareness. In addition, you can also access chapter versions of NPSG’s that detail Elements of Performance (EPs) for meeting goals and the rationale for why each goal is significant.
Although we do not personally endorse TJC, we appreciate and recognize that the NPSG’s are development with an intent to reduce harm to patients. Therefore, we can all appreciate that this information can be shared universally across all healthcare entities and programs regardless of accreditation affiliation or status. You can reference annual goals on their website The Joint Commission.
One of the primary goals that continues to require attention and focus is patient identification. In our experience, we find that methods used for patient identification methods may vary throughout a single organization. Predominantly, patients are asked to provide their name a date of birth to healthcare workers to aid in establishing proper identity. We encourage you to observe how your team identifies patients within your organization. It may be a good time to review your current policy as well as how staff are educated on proper patient identification methods. The consequences due to improper identification of a patient may include medication administration errors, unnecessary treatment for a diagnosis and unnecessary surgery being performed for example. These are just a few adverse events that may occur in addition to many others.
Another goal that continues to remain an area of concern addresses medication reconciliation. If medications are not reconciled in a structured and routine manner, patients may suffer from overdosing or experience serious and potentially fatal adverse reactions to medication. Medication reconciliation should always include medication name, purpose, dose and frequency. It is imperative that patients understand how to follow their prescribed medication regimen correctly.
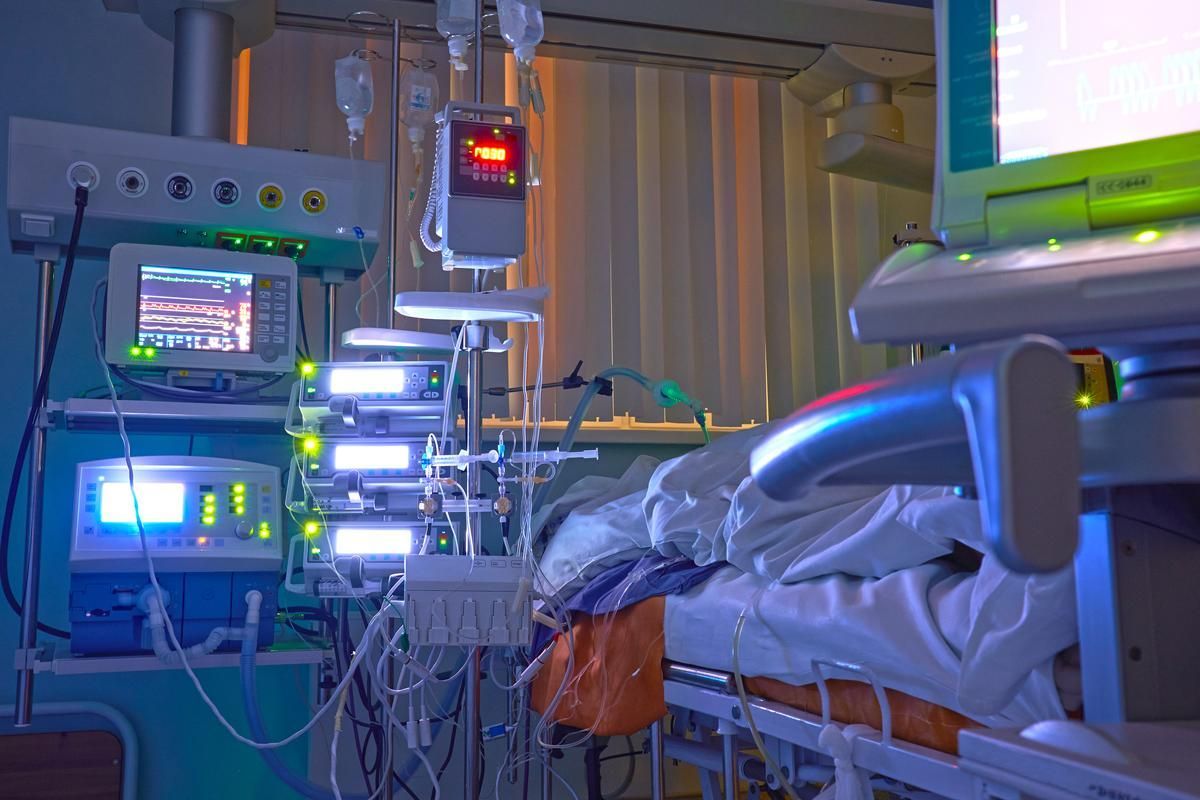
Alarms continue to remain an area of concern in healthcare organizations. Working in an environment, particularly with a significant amount of patient safety equipment in use is typically stressful for healthcare workers. Alarm fatigue occurs in these environments due to sensory overload as a result of hearing medical equipment alarm frequently. This often leads to unsafe silencing, changing alarm paraments or simply the shutting off of alarm associated with patient care sensors. Aversion to critical alarms remains a serious concern in healthcare today resulting in significant patient harm and death.
There continues to be a major focus on identifying and managing patients with suicidal ideation, reduction of healthcare associated infections and universal precautions to prevent wrong-site surgeries. Although specific NPSG’s will vary based on each type of healthcare program, the focus continues to be on risk reduction and improving patient safety.
We encourage organizations to take a brief look at TJC’s NPSG’s regardless of your organization’s accrediting body or accreditation status. We further encourage you to review your policies, protocols and training programs that address risk reduction relevant to the recurring and increasing concerns in patient care settings across the globe. Adverse events can easily lead to professional liability claims and revenue loss for healthcare organizations but more importantly significant harm to patients as well as death. The statistics continue to demonstrate that these problems remain prevalent and demand our attention. After all, the goal for all healthcare professionals working in this ever-changing and increasingly challenging industry should be to cause zero harm. This requires establishing, supporting and maintaining a culture of safety.
Our experts understand the challenges that all healthcare facilities are facing today. Using a customizable approach, we will help you navigate through even the toughest of challenges.
Whether you are in need of mock surveys, leadership training, corrective action plans or ongoing routine support services, we can help!
We pride ourselves on helping our clients achieve and maintain a status of excellence in the healthcare industry.
Be sure to browse
Our Website for a full list of services we provide.
Contact us today at +1 (800) 813-7117 to schedule a free consultation.